Examine inhabitants
The
ultimate examine inhabitants included 96 sufferers (45.8% females, age
70.6 ± 13.9 years). The stroke kind was ischemic in 88.5% of sufferers
and haemorrhagic in 11.5%. All sufferers introduced with a moderate-severe
hemiparesis. Predominant related neurological signs have been aphasia
(31.3%), gentle cognitive impairment (27.1%) and dysphagia (35.4%). Stroke
quantity was comparable for each aetiologies: 18.9 ± 40.4 ml for ischemic
occasions and 16.2 ± 18.2 ml for haemorrhagic lesions. Sufferers have been
admitted to the Neurorehabilitation Unit (NRB) after a imply of
7.3 ± 4.5 days from the stroke onset (index occasion). As much as 90% of
sufferers have been admitted to NRB inside 10 days from stroke onset. Desk 1 summarizes medical and demographic options of the examine inhabitants, whereas Desk 2 particulars medical and radiological options based on stroke subtype at hospital admission.
Prevalence of SII at NRB admission (T0) and elements related to SII
At NRB admission (T0), 15 out of 96 sufferers (15.6%) had a SII. Demographic options didn’t differ between SII and IC teams (Desk 1). Dysphagia was extra prevalent in sufferers with SII when in comparison with the IC group (66.7% vs. 29.6%, p = 0.007). The prevalence of comorbidities and voluptuary habits was comparable between SII and IC teams (Desk 1). NLR was equal to six.9 ± 1.9 within the SII group, and equal to 2.7 ± 0.9 within the IC group (p = 0.001).
Topics
with SII have been extra disabled when in comparison with IC group. Particularly,
the SII group was characterised by decrease useful independence (FIM
rating: SII = 54.2 ± 28.0 vs. IC = 75.5 ± 24.7, p = 0.007), extra extreme neurological incapacity (NIHSS rating: SII = 11.4 ± 6.2 vs. IC = 7.0 ± 4.1, p = 0.009), decrease performances within the actions of day by day dwelling (Barthel Index rating: SII = 21.7 ± 22.3 vs. IC = 44.6 ± 25.1, p = 0.001), and decrease motor performances (Tinetti rating: SII = 5.3 ± 8.2 vs. IC = 13.2 ± 9.9, p = 0.004). In response to the Hauser Ambulation Index, 52.4% within the IC group and 80% within the SII group (p = 0.453) wanted a wheelchair for many actions (Hauser Ambulation Index ≥ 7).
NLR positively correlated with age (r = 0.204, p = 0.046), stroke quantity (r = 0.269, p = 0.008), and NIHSS rating at T1 (r = 0.315, p = 0.002). As well as, it negatively correlated with the scores of the next scales, each at T0 and T1: FIM (T0, r = − 0.237, p = 0.020; T1, r = − 0.209, p = 0.041), Barthel Index (T0, r = − 0.329, p = 0.001; T1, r = − 0.206, p = 0.044) and Tinetti (T0, r = − 0.214, p = 0.036; T1, r = − 0.268, p = 0.008).
SII evolution over time
Blood cell counts have been obtainable from 83 sufferers at SU admission, and from 96 and 89 sufferers at T0 and T1,
respectively. Globally, SII confirmed a pattern towards discount over time.
The prevalence of SII was increased at SU admission when in comparison with NRB
admission (T0), (SU admission: 38.6%, T0: 15.6%, p = 0.001), and decreased upon discharge (T1: 6.7%, p = 0.047 vs. T0) (Fig. 1). SII decision occurred in 21 sufferers between SU admission and T0, and in 11 sufferers between T0 and T1. Of be aware, 5 sufferers who weren’t SII at SU admission grew to become so at later instances: 2 at T0 and three at T1.
Proportion
distribution of Stroke-Induced Immunosuppression (SII). Blood samples
to judge the presence of SII have been taken at SU admission (n = 83), NRB
admission (n = 96) and NRB discharge (n = 89). The prevalence of SII at
NRB admission was 15.6%, considerably decrease when in comparison with the acute
section (38.6%). Solely two sufferers acquired a primary analysis of SII at
NRB admission. The proportion of sufferers with SII at NRB discharge was
low (6.7%, p = 0.047); noteworthy, a late-onset SII was present in
three sufferers. SII: stroke-induced immunosuppression, outlined as a
neutrophil-to-lymphocyte ratio (NLR) ≥ 5. SU: Stroke Unit. NRB:
Neurorehabilitation Unit.
SII as a predictor of the rehabilitative end result
Practical independence measure – main end result
At T1, the useful independence (main end result) improved within the general examine inhabitants (FIM rating: T0 = 72.2 ± 26.3; T1:92.4 ± 27.9, issue TIME: p = 0.001). At T1 nonetheless, the SII group was nonetheless extra disabled than the IC group (SII = 75.3 ± 34.2 vs. IC = 95.6 ± 25.6, issue GROUP: p = 0.013). The extent of enchancment didn’t differ between SII and IC teams (interplay TIMExGROUP: p = 0.662) (Fig. 2, panel A).
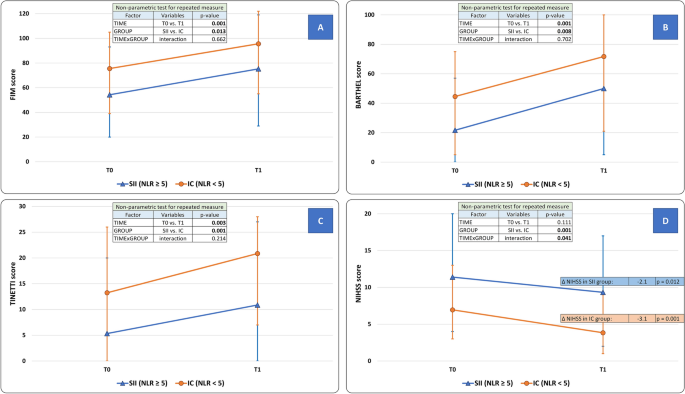
Modifications
of medical scales scores after the neurorehabilitative intervention in
Stroke-Induced Immunosuppression (SII) and Immunocompetent (IC) teams.
(Panel A) Practical Independence Measure (FIM) rating; (Panel B) Barthel Index rating; (Panel C) Tinetti stability scale rating; (Panel D)
Nationwide Institutes of Well being Stroke Scale (NIHSS) rating. FIM rating
(main end result), Barthel Index, and Tinetti scale improved on the finish
of the rehabilitation interval (issue TIME, p < 0.050). For these parameters, the presence of SII was an impartial predictor of general incapacity (issue GROUP, p < 0.050), though it didn’t have an effect on the diploma of enchancment (interplay TIMExGROUP, p > 0.050).
Just for NIHSS rating, SII qualifies as a damaging predictor of the
rehabilitative intervention (interplay TIMExGROUP, p < 0.035) in addition to of the general end result (issue GROUP, p = 0.001).
Statistical evaluation: non-parametric check for repeated measures: issue
“TIME” is expression of the efficacy of the rehabilitative therapy in
the general inhabitants; issue “GROUP” is expression of the comparability
between SII and IC teams throughout all time-points; a big
TIMExGROUP interplay is expression of a distinction between SII and IC
teams in addition to of a distinction within the diploma of enchancment between
SII and IC teams over time. The extent of significance was corrected for
“Age”, “Intercourse”, “Time from stroke to NRB admission”, and “Stroke quantity”.
SII: stroke-induced immunosuppression, outlined as a neutrophil to
lymphocyte ratio (NLR) ≥ 5. SU: Stroke Unit. NRB: Neurorehabilitation
Unit. IC: Immunocompetent sufferers.
FIM rating at discharge (T1) negatively correlated with age (r = − 0.425; p = 0.001), period of hospitalization (r = − 0.448; p = 0.001), and vascular lesion extension (r = − 0.323; p = 0.001). Variations in FIM rating at T1 have been discovered primarily based on the presence of aphasia at T0 (p = 0.015), presence of a minimum of one infectious complication (p = 0.001) or stress ulcers (p = 0.002) throughout hospitalization, and optimistic medical historical past of atrial fibrillation (p = 0.022), myocardial infarction (p = 0.028), or alcohol abuse (p = 0.023).
After
statistical correction for intercourse, stroke quantity, period of
hospitalization, days from stroke onset (index occasion) to NRB admission,
and sort of stroke (ischemic or haemorragic), the linear regression
demonstrated that FIM rating at T1 was related to the NLR (β − 6.56 [− 11.9 to − 1.2]; p = 0.018), age (β − 0.58 [− 1.0 to − 0.2]; p = 0.010), and presence of stress ulcers (− 26.9 [− 49.8 to − 4.1]; p = 0.023) (Desk 3). The adjusted R2 was 0.568.
Performances within the actions of day by day dwelling
At T1, the performances within the actions of day by day dwelling improved within the general examine inhabitants (Barthel Index rating: T0 = 40.9 ± 25.9; T1 = 68.3 ± 30.2, issue TIME: p = 0.001). The SII group was nonetheless extra disabled at T1 when in comparison with IC group (IC: 71.7 ± 27.3; SII: 50.0 ± 39.0, issue GROUP: p = 0.008). The extent of enchancment didn’t differ between SII and IC teams (interplay TIMExGROUP: p = 0.702) (Fig. 2, panel B).
Motor performances
At T1, motor performances based on the Tinetti scale rating improved within the general examine inhabitants (T0 = 12.0 ± 10.0; T1 = 19.3 ± 9.2, issue TIME: p = 0.003). SII group was nonetheless extra disabled at T1 when in comparison with IC group (IC: 20.8 ± 7.9; SII: 10.9 ± 11.2, issue GROUP: p = 0.001). The speed of enchancment didn’t differ between SII and IC teams (interplay TIMExGROUP: p = 0.214) (Fig. 2, panel C). Relating to Hauser Ambulation Index, SII group was nonetheless extra disabled at T1 when in comparison with IC group. Certainly, at T1 53.4% in SII group versus solely 19% in IC group (p = 0.031) wanted a wheelchair for many actions (Hauser rating ≥ 7).
Neurological incapacity
Each teams achieved a big enchancment on this parameter: IC group (T0 = 6.9 ± 4.2 vs. T1 = 3.8 ± 3.1, ΔNIHSS: − 3.1 ± 2.5, p = 0.001); SII group (T0 = 11.4 ± 6.2 vs. T1 = 9.3 ± 5.3, ΔNIHSS: − 2.1 ± 2.3, p = 0.012). The speed of enchancment was nonetheless extra pronounced within the IC group (interplay TIMExGROUP: p = 0.041). The general neurological incapacity was extra extreme in SII group (issue GROUP: p = 0.001) (Fig. 2, panel D).
Length of hospitalization, vacation spot at discharge and issues
The period of hospitalization didn’t differ between teams (IC: 46.4 ± 15.1; SII = 51.1 ± 13.8 days, p = 0.081).
In contrast, a decrease share of sufferers within the SII group (7/15,
46.7%) have been discharged at residence when in comparison with the IC group (64/81,
79.0%) (p = 0.032) (Supplementary Desk 1).
Throughout
SU hospitalization, 22 sufferers had an infectious complication. This
was related to presence of SII at SU admission as extra sufferers
with SII had a historical past of infectious issues throughout SU
hospitalization (13/32, 40.6%) when in comparison with IC sufferers (9/51,
17.6%, p = 0.038). Conversely, infectious issues occurring
in SU weren’t related to the presence of SII at NRB admission.
Certainly, at NRB admission solely 3 sufferers with SII had a historical past of
infectious issues throughout SU hospitalization (3/14, 21.4%)
in comparison with 19 within the IC group (19/79, 42.1%, p = 0.343).
On
the opposite hand, the proportion of sufferers with a minimum of one infectious
complication throughout NRB hospitalization was increased within the sufferers with
SII at NRB admission (12/15, 80%) when in comparison with the IC group (21/81,
25.9%) (p = 0.001); this distinction was primarily defined by the prevalence of urinary tract infections (IC: 18.5%; SII: 53.3%; p = 0.007) (Supplementary Desk 1). The incidence of different non-infectious issues didn’t differ between examine teams.